Imagine no longer having to pinch your skin for multiple injections every single day. For many people living with type 1 diabetes, the transition to insulin pump therapy is exactly that-a liberation from the needle. Instead of relying on several daily shots of long-acting and short-acting insulin, a pump provides a steady stream of insulin, mimicking how a healthy pancreas works. While it sounds like a magic fix, it's actually a sophisticated tool that requires a learning curve and a commitment to technical management.
If you're tired of the "rollercoaster" effect-where your blood sugar swings wildly from high to low-you might be wondering if this technology is right for you. The reality is that while pumps can drastically lower your HbA1c and give you more freedom with your meals, they also introduce new risks, like device failure or site infections. This guide breaks down what actually happens when you switch, the trade-offs you'll face, and how to get started without feeling overwhelmed.
The Bottom Line on Insulin Pumps
Before getting into the weeds, here is the quick take on whether a pump is worth the effort:
- The Big Win: Better blood glucose stability and significantly fewer nighttime lows.
- The Trade-off: You trade needles for a wearable device and a set of alarms.
- The Requirement: You need a baseline ability to calculate carbs and a willingness to monitor your levels closely.
- The Goal: Lowering your HbA1c and gaining flexibility in your daily schedule.
How Insulin Pumps Actually Work
At its core, Insulin Pump Therapy is a method of continuous subcutaneous insulin infusion (CSII). Unlike multiple daily injections (MDI), where you take one long-acting dose and several short-acting doses, a pump uses only rapid-acting insulin. It delivers this insulin in two ways: a constant "basal" rate that runs 24/7 and "bolus" doses that you trigger manually when you eat or need to correct a high reading.
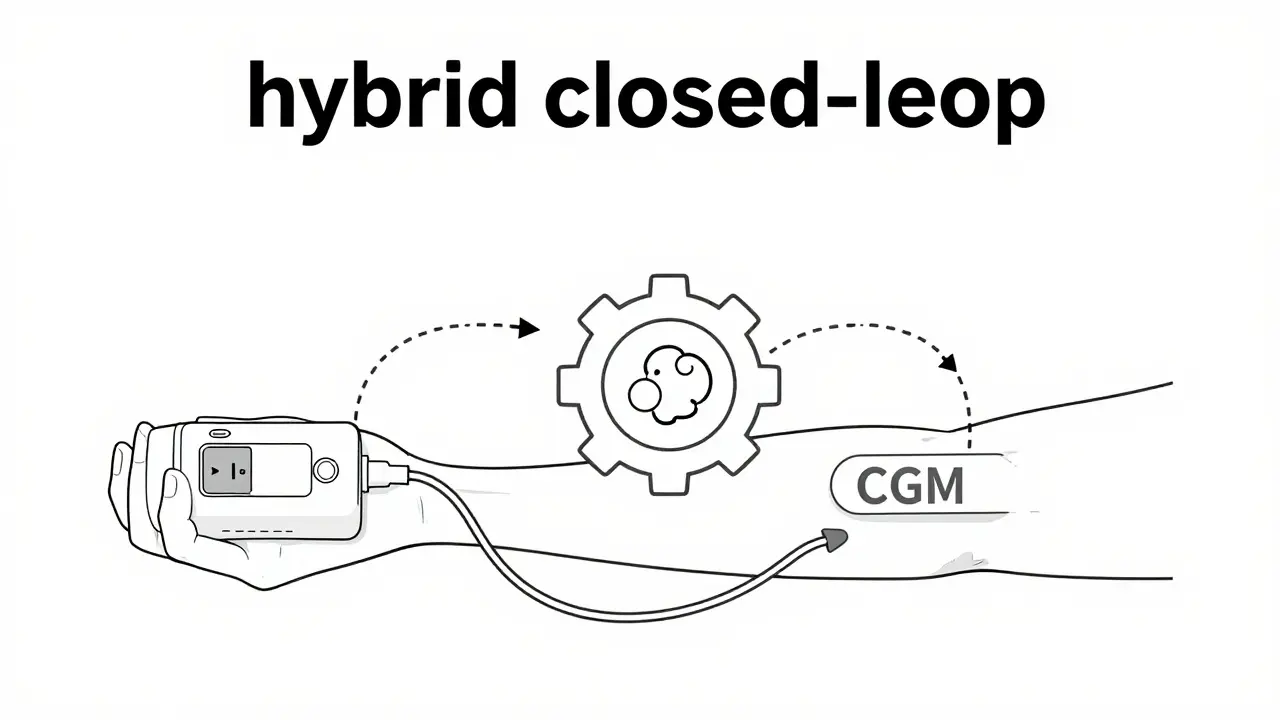
Modern systems have evolved into Automated Insulin Delivery (AID) systems. These pumps talk to a Continuous Glucose Monitor (CGM)-a sensor under your skin that tracks glucose every few minutes. The pump then uses an algorithm to automatically increase or decrease the insulin flow based on where your sugar is heading. It's essentially a "hybrid closed-loop" system that does a lot of the heavy lifting for you.
Depending on your lifestyle, you'll likely choose between two main designs:
- Tethered Pumps: A small device worn on the belt or in a pocket, connected to the body via a thin plastic tube. Examples include the Medtronic MiniMed 780G and the Tandem t:slim X2.
- Patch Pumps: Tubeless pods that stick directly to your skin. The Omnipod 5 is the leader here, offering a more discreet profile and waterproof capabilities that are great for swimmers or active kids.
The Pros: Why People Make the Switch
The most immediate benefit is the precision. While a syringe allows for basic dosing, a pump can deliver increments as small as 0.01 units. This is a game-changer for people who are highly sensitive to insulin or children who require tiny doses. Research shows this precision pays off; a 2022 meta-analysis found that pump users had HbA1c levels around 8.3%, compared to 9.2% for those on injections.
Then there's the "sleep factor." One of the most terrifying parts of type 1 diabetes is nocturnal hypoglycemia-the dangerous lows that happen while you're asleep. Because pumps can adjust basal rates and some can even suspend insulin delivery if they predict a drop, users often see a 32% reduction in these overnight episodes. This means better sleep and less anxiety for both the patient and their family.
Finally, there is the flexibility. If you want to go to a movie or take a nap, you don't have to time your long-acting insulin perfectly. You can simply adjust your settings on the fly. Many users report that the ability to change their meal timing without worrying about "insulin stacking" from a long-acting dose significantly improves their quality of life.
The Cons: The Hidden Challenges
It isn't all smooth sailing. The biggest risk with a pump is that it is a single point of failure. If a tube kinks, a site becomes infected, or the battery dies, you stop receiving all your insulin. Since pumps use rapid-acting insulin, you can enter Diabetic Ketoacidosis (DKA) very quickly-sometimes within 4 to 6 hours of a delivery failure. This is why pump users must always carry backup insulin pens.
Then there's the "alarm fatigue." Your pump will beep, vibrate, or scream when you're low, high, or the reservoir is empty. While these are life-saving, they can become a source of stress and social awkwardness. Additionally, about 45% of users experience skin irritation at the infusion site, which requires rotating the site every few days to avoid scarring or lipohypertrophy.
There is also a cognitive load. A pump isn't a "set and forget" device. You have to program your insulin-to-carb ratios and correction factors. If you enter the wrong number of carbs into the pump, you get the wrong dose of insulin, which can lead to a severe hypoglycemic event.
| Feature | Insulin Pump (CSII) | Injections (MDI) |
|---|---|---|
| Insulin Type | Rapid-acting only | Long-acting + Rapid-acting |
| Precision | Very High (0.01 unit increments) | Moderate (Syringe/Pen limits) |
| Nighttime Lows | Lower risk (Auto-adjust/Suspend) | Higher risk (Fixed basal dose) |
| Daily Burden | Device management & site changes | Multiple daily needle sticks |
| Risk of Failure | Technical failure can lead to rapid DKA | Forgotten dose leads to slower rise in sugar |
Getting Started: Your Onboarding Roadmap
You can't just buy a pump and start using it tomorrow. The transition usually takes 2 to 4 weeks of structured education. Most clinics will put you through 3 to 5 specialized sessions to ensure you're ready. If you jump in too fast, the risk of dosing errors is high.
First, your healthcare provider will assess your readiness. Do you have the dexterity to change a site? Can you hear the alarms? Most importantly, can you accurately calculate your Insulin-to-Carbohydrate Ratio (ICR)? You'll need to know exactly how many grams of carbs one unit of insulin covers for your specific body.
Once the hardware is set up, you'll enter the "tuning phase." This is where you and your doctor refine your basal rates. You might find that you need more insulin at 4 AM (the dawn phenomenon) and less at 2 PM. This titration period is where the real magic happens, as you strip away the guesswork of MDI.
Pro tip: Don't ditch your glucose meter immediately. Even if you have a CGM, you'll need a finger-stick meter to calibrate the sensor or double-check a reading if the pump says you're stable but you feel shaky. This "trust but verify" approach is the only way to safely manage the technology.
Who is a Good Candidate?
Pumps are fantastic, but they aren't for everyone. You are likely a great candidate if:
- Your A1C remains above 7.5% despite your best efforts with injections.
- You experience "hypoglycemia unawareness," meaning you don't feel the signs of a low until it's dangerous.
- You have highly variable glucose levels that make it impossible to predict your needs.
- You have a job or hobby (like swimming or long-distance hiking) that makes multiple injections impractical.
On the flip side, some people find pumps frustrating. If you have significant anxiety about technology or a history of eating disorders that make strict carb counting difficult, the cognitive demand of a pump might be too high. Some people simply prefer the simplicity of a pen and a meter, and that's perfectly okay.
How much does an insulin pump cost?
The pump itself typically ranges from $5,000 to $7,000, with annual supplies (reservoirs, infusion sets) costing another $3,000 to $5,000. However, many insurance plans, Medicare, and Medicaid cover a large portion of these costs, often leaving the user with copays between $100 and $500 after deductibles are met.
Does it hurt to wear a pump?
The initial insertion of the cannula (the small tube under the skin) feels like a quick pinch, similar to an injection. Most people find that wearing the pump is actually less painful over time because they aren't poking themselves 4-6 times a day. Some users do experience skin irritation from the adhesive, which can be managed with barrier wipes.
Can I shower or swim with an insulin pump?
It depends on the model. Tubeless patch pumps like the Omnipod 5 are designed to be waterproof up to 3 meters for 30 minutes. Tethered pumps may require you to disconnect the tubing before swimming or taking a bath to avoid water entering the system or the device becoming damaged.
What happens if the pump fails?
If a pump fails, you stop receiving basal insulin immediately. Because you are using rapid-acting insulin, your blood sugar can spike quickly, and ketones can build up. You must immediately switch to your backup insulin pens (long-acting and short-acting) and monitor your ketones. If you can't get your sugars down, seek emergency medical care to prevent DKA.
How often do I have to change the pump site?
Most infusion sets need to be changed every 2 to 3 days. This prevents infection and ensures the insulin is absorbed efficiently. If you leave a site in too long, you may develop lumps of fat or scar tissue (lipohypertrophy), which makes insulin absorption unpredictable.
Next Steps and Troubleshooting
If you're ready to move forward, start by asking your endocrinologist for a technology assessment. Don't just ask for "a pump"; ask which system matches your lifestyle. If you're a swimmer, look at patch pumps. If you want the most advanced automated adjustments, look at the latest AID systems.
For New Users: Expect a few "bad' days during the first month. You might over-bolus or struggle with the site placement. This is normal. Keep a detailed log of your glucose readings and what you ate; this data is the only way your doctor can help you tune your basal rates.
For Experienced Users: If you're feeling "alarm fatigue," talk to your provider about adjusting your alert thresholds. You can often silence non-critical alerts or change the notification style to be less intrusive without sacrificing safety.


Write a comment